Introduction
Frostbite is a serious condition caused by exposure of the skin and underlying tissues to extreme cold. While ice packs are a popular method for pain relief and reducing swelling, their improper use can lead to frostbite from ice pack. It’s essential to understand the risks involved with using ice in therapy and how to use it safely.
In this article, we will explore the causes and symptoms of frostbite from ice pack, provide safe guidelines for their use, and discuss effective treatment options if frostbite occurs. Knowing how to apply ice correctly can ensure you benefit from its therapeutic effects without the dangers of frostbite harming your skin.
Understanding Frostbite: Causes and Risk Factors
Frostbite happens when skin and tissues freeze due to prolonged exposure to cold temperatures, often exacerbated by direct contact with ice packs. Here are some key causes and risk factors contributing to frostbite:
Temperature
The primary reason frostbite can occur from ice packs is the temperature at which they operate. Ice packs maintain temperatures around 32°F (0°C) or lower. When applied directly to the skin, they can significantly reduce skin temperature and cause tissue damage if not used properly.
Duration of Exposure
Using an ice pack for longer than recommended significantly increases your risk of frostbite. Experts typically advise using ice packs for no longer than 20 minutes at a time. Prolonged exposure can quickly elevate the risk of frostbite, especially if the skin is already sensitive.
Skin Condition
Certain underlying skin conditions, such as diabetes or poor circulation, can enhance the likelihood of frostbite. Individuals with these conditions may have impaired blood flow, making them more susceptible to cold injury.
Moisture
Moisture facilitates faster heat transfer, increasing the risk of frostbite. If the skin or the ice pack itself is wet, the sensation of cold can intensify, which may lead to frostbite more quickly than if the skin were dry.
Individual Factors
Different individuals may have varying tolerances to cold. Factors like age, gender, and overall health play a role in susceptibility to frostbite. Older individuals or those with pre-existing health conditions may be more vulnerable.
By understanding these factors, you can take proactive measures to minimize the risk involved with using ice packs for injuries.
Symptoms of Frostbite From Ice Pack
Recognizing the early signs of frostbite is vital for preventing further injury. Symptoms typically develop in stages, allowing individuals to gauge severity effectively.
Stage 1: Initial Symptoms
The initial symptoms of frostbite may include:
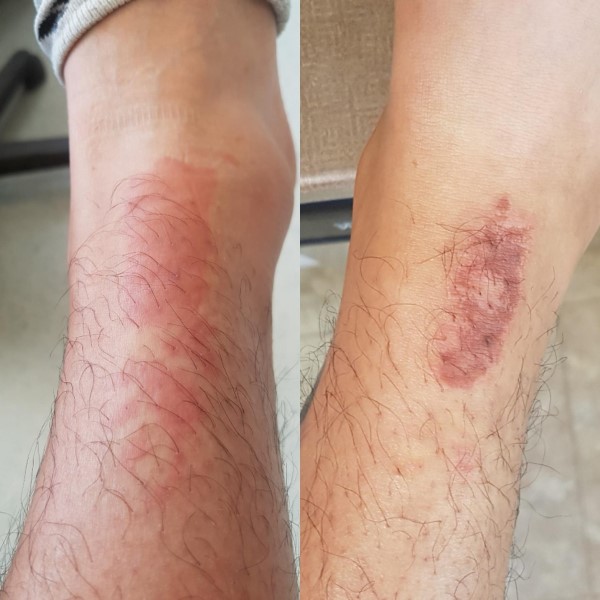
Redness
When frostbite begins to develop, one of the earliest signs is the reddening of the skin in the affected area. This redness is a result of increased blood flow to the skin, which occurs as the body attempts to protect itself from the cold. Initially, this vibrant red hue indicates inflammation, serving as a warning signal that the skin has been affected by low temperatures. This response is a part of the body’s natural defense mechanisms, attempting to keep the deeper tissues warm. However, if exposure continues, the redness may turn into a paler or whitish color as blood vessels constrict to minimize heat loss, indicating a progression toward frostbite. Recognizing this initial redness is vital, as it can prompt timely intervention to avoid more severe tissue damage.
Cold Sensation
Along with the visible changes in color, individuals experiencing frostbite commonly report a notable cold sensation in the affected area. This cooling occurs because the tissues are losing heat at an accelerated rate due to the exposure to freezing conditions. The affected area may feel significantly colder than the surrounding skin, reflecting a decrease in temperature that can lead to painful sensations as the body reacts defensively. The loss of warmth signals that blood flow to the extremities is diminishing, and as a consequence, the skin becomes increasingly vulnerable to damage. This stark temperature difference serves as an alert, emphasizing the importance of immediate action to prevent further complications, including severe frostbite and tissue death.
Tingling or Stinging
As frostbite progresses, individuals often report tingling or a stinging sensation in the affected area, commonly referred to as a “pins-and-needles” feeling. This occurs as the body’s blood flow slows and the nerves become compromised due to the cold. Initially, this tingling may be mild, but it can intensify as the condition worsens. This sensation is an indication of nerve response; it signifies that the nerves are reacting to the cold and the reduction in blood supply. While some may perceive this feeling as a temporary inconvenience, it is essential to understand that persistent tingling can be a warning sign of progressing frostbite. Recognizing this symptom early on can lead to actions that prevent further damage and facilitate quicker recovery.
Stage 2: Moderate Symptoms
As frostbite progresses, symptoms may worsen:
- White or Pale Skin: The affected area may become white or pale as blood flow decreases.
- Numbness: A loss of sensation often sets in, making it difficult to feel pain in the area.
- Swelling: The skin may start to swell, indicating that tissues are compromised.
Stage 3: Severe Symptoms
In severe cases of frostbite, symptoms become even more alarming:
- Hard or Waxy Skin: The skin may feel stiff and hard to the touch, indicating significant freezing.
- Blistering: Blisters may appear as tissues begin to thaw, signaling that medical attention is essential.
- Blue or Purple Color: The skin can take on a bluish or purplish color, indicating a severe lack of blood flow.
Understanding these symptoms can help individuals respond adequately before severe damage occurs.
Safe Guidelines for Using Ice Packs
To minimize the risk of frostbite from ice packs, follow these essential guidelines when using cold therapy:
1. Use a Barrier
Always place a thin cloth, towel, or another protective barrier between the ice pack and your skin. This barrier reduces the cold’s direct impact, helping to mitigate the risk of frostbite while still providing therapeutic benefits.
2. Limit Exposure Time
To avoid frostbite, ice packs should be applied for a maximum of 20 minutes at a time. After this duration, remove the ice pack and allow the skin to return to its normal temperature for at least 30-60 minutes before applying it again.
3. Monitor Your Skin
Regularly check the skin under the ice pack while using it. If you notice any signs of redness, discoloration, or other alarming changes, remove the ice pack immediately. Prompt action can prevent frostbite.
4. Keep the Rest of Your Body Warm
When using an ice pack, ensure the remainder of your body is warm. Wearing warm clothing and maintaining overall body temperature helps prevent further heat loss, minimizing frostbite risk in unaffected areas.
5. Be Cautious with Preexisting Conditions
If you have health issues such as cardiovascular problems, diabetes, or peripheral neuropathy, consult a healthcare professional before using ice packs. Special considerations may be necessary to ensure your safety.
6. Avoid Using Ice Packs on Wet Skin
Moisture enhances the freezing capability of ice. Before applying an ice pack, ensure that your skin is dry. Additionally, ensure the ice pack itself is not leaking or wet.
Sticking to these guidelines will greatly improve the safety and effectiveness of your cold therapy treatment.
Common Questions About Frostbite From Ice Pack
How Do You Treat Frostbite From an Ice Pack?
If frostbite is suspected from ice pack usage, the affected area should be gradually warmed. Remove the ice pack immediately and soak the area in warm, not hot, water for roughly 30 minutes. Avoid direct heat sources, as these can lead to burns.
How Quickly Can You Get Frostbite From an Ice Pack?
Frostbite can occur within 20-30 minutes if an ice pack is placed directly on the skin without a barrier. The duration can be quicker in particularly cold conditions or with wet skin.
How Do You Know If You Have an Ice Pack Burn?
Ice pack burns can occur when the skin becomes excessively cold. Symptoms may include redness, swelling, blistering, and a burning sensation. If you suspect an ice pack burn, stop using it and let the area warm up gradually.
What Does the First Stage of Frostbite Feel Like?
In the first stage of frostbite, you may feel coldness in the affected area, accompanied by tingling or stinging sensations. The skin may initially appear red but can change to a pale or white color as the situation progresses.
Conclusion: Importance of Safety in Cold Therapy
In summary, understanding how to safely use an ice pack can prevent frostbite and ensure effective treatment for injuries. While ice packs offer valuable benefits for pain management and swelling, improper usage can lead to serious complications. By adhering to the guidelines outlined in this article, you can safeguard your skin and health while reaping the benefits of cold therapy.
Always remember the importance of monitoring your skin, using barriers, and limiting exposure time. Increasing awareness of these practices will enhance your recovery experience and minimize complications like frostbite from ice pack. With proper precautions, you can safely enjoy the therapeutic effects of ice packs while protecting your skin from harm. Embrace your cold therapy with confidence; it can be a powerful tool in your healing journey.