The Science Behind Cold Therapy and Healing
Understanding the immediate physiological response to injury is crucial for effective treatment. When soft tissue sustains damage, the body initiates a complex inflammatory process. Consequently, blood vessels dilate to allow essential nutrients and white blood cells to reach the injured site. While this inflammation is a natural part of healing, it often results in significant pain and swelling. Therefore, applying ice, or cryotherapy, serves as a primary intervention to manage these acute symptoms. The cold temperature causes vasoconstriction, which narrows the blood vessels. This process reduces blood flow to the affected area, thereby limiting the accumulation of fluid that causes swelling. Many athletes and active individuals often ask how long should you ice an injury to achieve these benefits without causing harm.
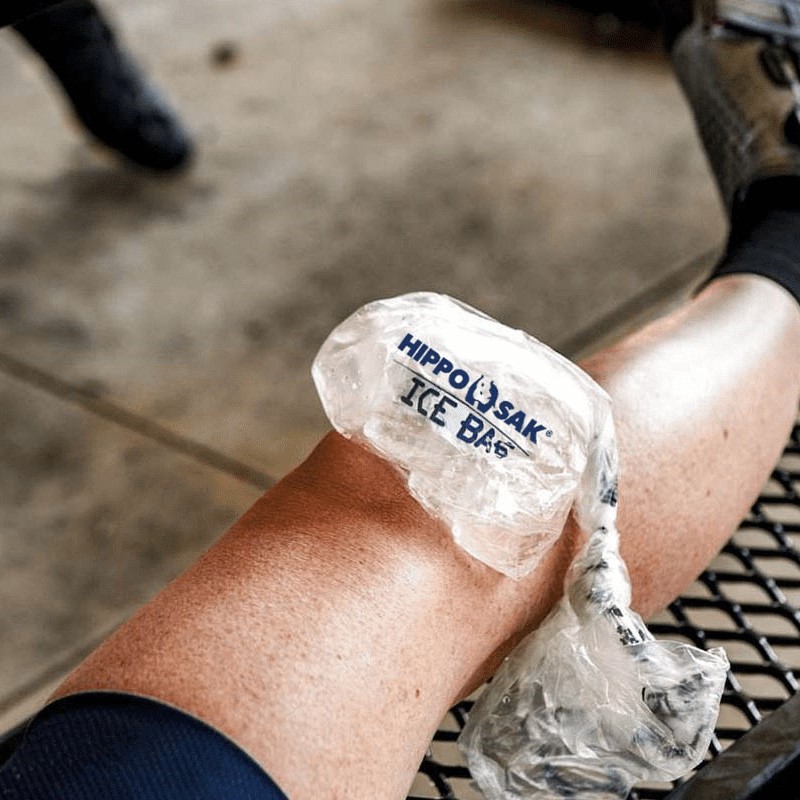
Moreover, the application of cold acts as a local anesthetic. It slows down nerve transmission rates, which effectively numbs the pain. This analgesic effect allows patients to move the injured limb more comfortably, facilitating early mobilization. However, one must approach this therapy with caution. Prolonged exposure to cold can damage the skin and underlying tissues. Thus, finding the balance between therapeutic benefit and tissue safety is essential. We must recognize that ice is a tool, not a cure-all solution. It temporarily interrupts the inflammatory cascade but does not entirely stop the necessary healing process. By grasping the basic science of vasoconstriction and metabolic reduction, patients can use ice more effectively. This knowledge forms the foundation for the specific timing guidelines discussed in the following sections.
Determining the Optimal Duration for Icing
Establishing a specific timeframe for cold application is vital for safety and efficacy. Medical professionals generally recommend a standard duration for applying cold therapy. Typically, you should apply ice for sessions lasting between 15 and 20 minutes. This timeframe is sufficient to penetrate deep tissues and induce vasoconstriction. However, it is short enough to prevent frostbite or nerve damage. Consequently, the question of how long should you ice an injury becomes a matter of precision rather than estimation. If you ice for less than 10 minutes, the cold may not penetrate deeply enough to affect the underlying muscle or joint. Conversely, exceeding the 20-minute threshold poses significant risks to your skin and nerves.
Furthermore, consistency plays a pivotal role in the recovery process. You should repeat these 15 to 20-minute sessions every two to three hours during the initial 48 to 72 hours after the injury. This intermittent application creates a “pumping” action in the blood vessels. First, the cold constricts the vessels. Then, when you remove the ice, the vessels dilate. This cycle helps flush out metabolic waste products from the injured area. It is important to note that individual physiology can influence the ideal duration. Individuals with thinner skin or less body fat in the injured area may need to reduce the time to 10 or 15 minutes. Conversely, those with more muscle mass might require the full 20 minutes to feel the effects. Always monitor the skin’s appearance throughout the session. If the skin turns bright red or feels burning, you should remove the ice immediately. Adhering to these timing guidelines ensures that you maximize pain relief while minimizing potential harm.
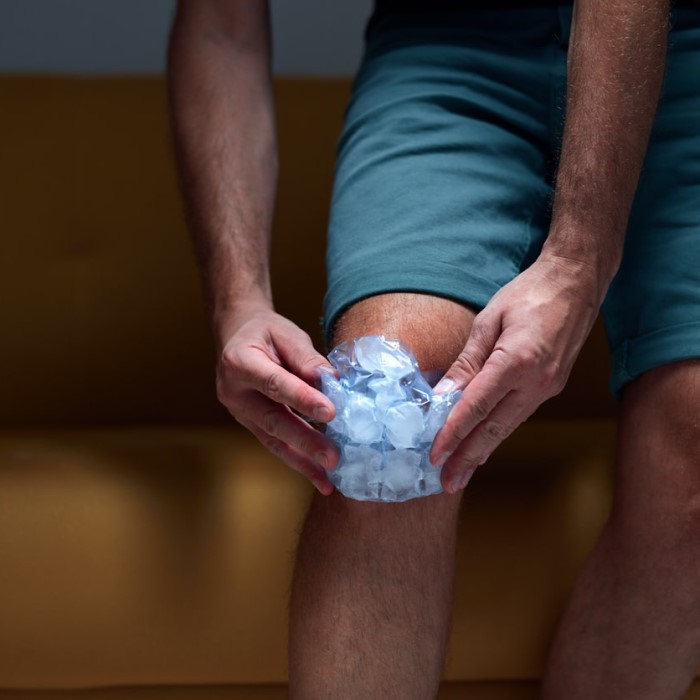
Recognizing the Critical Warning Signs to Stop
While cold therapy offers numerous benefits, over-icing can lead to serious complications. Therefore, you must remain vigilant for specific indicators that signal when to stop. The most immediate sign is a change in sensation. Initially, you will feel cold, followed by a burning sensation, and finally numbness. Once the area feels numb, the primary therapeutic goal has been achieved. Keeping the ice on past the point of numbness provides no additional benefit. In fact, it increases the risk of tissue damage. Consequently, if you ask yourself how long should you ice an injury, the answer often lies in your sensory feedback rather than the clock.
In addition to sensory changes, visual cues are equally important. The skin should not turn stark white or appear waxy. These changes indicate that ice crystals may be forming within the tissue, which is a precursor to frostbite. Furthermore, you should check for skin mottling or purple discoloration. These visual signs suggest that blood flow has been restricted for too long, potentially causing damage to the superficial capillaries. Another critical warning sign is pain that worsens instead of subsides. While the initial cold application can feel uncomfortable, it should transition into relief. If the pain spikes or throbs intensely, the body is signaling distress. You should also pay attention to the surrounding tissue. If areas far from the injury site become numb or discolored, the cold is spreading too broadly. In such cases, remove the ice pack instantly. By respecting these warning signs, you protect your body from the adverse effects of excessive cold exposure, ensuring a safe recovery path.
Common Mistakes to Avoid During Application
Many individuals unintentionally make errors when applying cold therapy, which can hinder recovery. One of the most frequent mistakes is applying ice directly to the skin. Direct contact creates a high risk of frostbite and ice burns. Therefore, you should always place a thin barrier between the ice pack and your skin. A damp towel or a pillowcase works perfectly for this purpose. This barrier allows the cold to penetrate while protecting the surface of the skin. Another common error involves falling asleep with the ice pack in place. Without conscious monitoring, it is easy to exceed the recommended time limits. This oversight can lead to serious nerve damage or frostbite.
Furthermore, many people believe that “more is better” when it comes to pain relief. They might ice for an hour straight, thinking it will help more than a short session. However, this approach is counterproductive. Prolonged icing can actually cause the body to increase blood flow in an attempt to warm the area, leading to a rebound effect. This phenomenon increases swelling rather than reducing it. Additionally, some individuals use ice packs that are too heavy. Heavy bags of frozen vegetables or large ice blocks can place unwanted pressure on the injury. This pressure can compress tissues and increase pain. Instead, use lightweight gel packs or bags of crushed ice that conform to the body’s contours. Understanding these pitfalls helps you refine your approach to injury management. By avoiding these mistakes, you ensure that your cryotherapy sessions remain safe and effective.
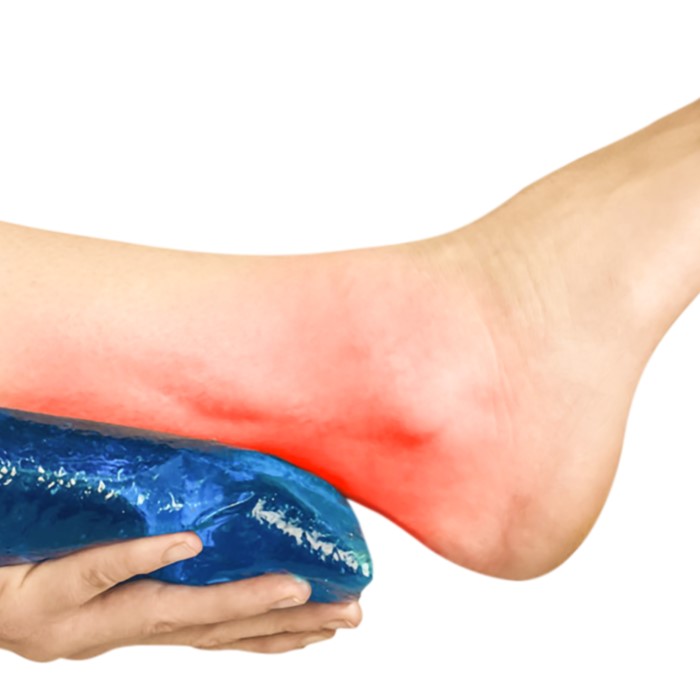
Understanding the Different Stages of Healing
The body heals injuries in distinct phases, and your treatment strategy should evolve accordingly. The first stage is the acute inflammatory phase, which lasts approximately 72 hours. During this initial period, the injured site experiences swelling, redness, and heat. This is the prime time for ice application. Cold therapy effectively manages the inflammatory response and controls pain. However, once the acute phase passes, the body enters the sub-acute phase. This stage focuses on repair and regeneration. New blood vessels form, and collagen fibers begin to bridge the gap in the damaged tissue. At this point, the need for ice diminishes significantly. While you might still use ice after intense physical therapy sessions, constant icing is no longer necessary.
Following the sub-acute phase is the remodeling phase. This final stage can last for months or even years. The body strengthens the new tissue and reorganizes collagen fibers to match the original structure. During this time, the focus shifts from inflammation control to mobility and strength. Consequently, applying ice is typically reserved for flare-ups or post-workout soreness. It is rarely used as a primary treatment modality during this late stage. Understanding these timelines helps you transition your treatment plan. Clinging to ice therapy when the injury has moved into the repair or remodeling stages can actually slow down healing. The cold reduces blood flow, which is essential for delivering the nutrients required for tissue repair. Therefore, knowing when to stop icing is just as important as knowing how to start. You must align your treatment with your body’s current physiological needs.
The R.I.C.E. Protocol and Its Role
For decades, the R.I.C.E. acronym has served as the gold standard for acute injury management. This acronym stands for Rest, Ice, Compression, and Elevation. Each component plays a synergistic role in recovery. Rest protects the injured tissue from further damage. It allows the healing process to begin without interference. Ice, as discussed, controls pain and limits swelling through vasoconstriction. Compression involves applying an elastic bandage to the area. This pressure helps limit the space available for swelling to develop. Finally, elevation raises the injured limb above the level of the heart. This position uses gravity to drain excess fluid away from the injury site. Together, these four elements create a comprehensive treatment plan.
However, recent medical debates have questioned the “Rest” and “Ice” components. Some experts suggest that complete rest can lead to joint stiffness and muscle atrophy. They now advocate for “P.E.A.C.E. and L.O.V.E.,” a newer acronym that emphasizes education and load management. Despite this evolution, ice remains a useful tool for pain management in the very early stages. It should not be viewed as a standalone cure but as part of a broader strategy. For instance, when you apply ice, you should simultaneously elevate the limb. This combination maximizes the reduction of edema. Similarly, compression should be applied firmly but not tightly enough to cut off circulation. You must check for distal pulses or capillary refill to ensure safety. By integrating these methods, you address the injury from multiple angles. This holistic approach accelerates recovery far more effectively than ice alone. It ensures that you are not just masking the pain but actively facilitating the healing process.

Alternatives and Supplements to Ice Therapy
While ice is a powerful tool, it is not the only option for managing injuries. Heat therapy serves as a valuable counterpart to cold therapy. However, heat is generally not appropriate during the acute inflammatory phase. Applying heat to a fresh injury will increase blood flow, which can exacerbate swelling and pain. Instead, heat is best used during the later stages of healing. It relaxes tight muscles and increases tissue elasticity, which aids in rehabilitation. Consequently, knowing when to switch from ice to heat is a critical skill. Alternating between hot and cold, known as contrast therapy, is another technique. This method creates a pumping action that stimulates blood flow and reduces congestion in the area.
Additionally, non-thermal modalities can provide relief. Over-the-counter anti-inflammatory medications, such as ibuprofen, can help manage pain and inflammation from the inside. Topical analgesics like creams and gels offer localized pain relief without the temperature change. Gentle movement is also a potent supplement to icing. While you should avoid strenuous activity, gentle range-of-motion exercises prevents stiffness. These movements help align collagen fibers and prevent scar tissue from forming too densely. Massage is another effective technique for later stages of recovery. It helps break up adhesions and improve circulation to the healing tissues. By combining these various modalities, you create a dynamic recovery plan. You do not rely solely on one method. Instead, you use a toolkit of strategies to support your body’s natural healing capabilities. This multi-faceted approach leads to stronger, more resilient tissue repair.
Frequently Asked Questions About Icing Injuries
Many patients still have lingering questions regarding the specifics of cryotherapy. Addressing these common queries helps clarify best practices for injury management. Here are the answers to four frequently asked questions.
What is the 20 20 20 rule for ice and heat?
This rule is a helpful guideline for contrast therapy. You apply ice for 20 minutes, then remove it. Afterward, you wait 20 minutes to let the tissues return to normal temperature. Finally, you apply heat for 20 minutes. This cycle helps stimulate circulation and reduce congestion. However, this method is typically reserved for sub-acute injuries, not fresh, acute injuries.
How long is too long to ice an injury?
Any application exceeding 20 minutes at a time is generally considered too long. Furthermore, icing for multiple hours consecutively can cause severe tissue damage. If you leave ice on for 30 minutes or more, you risk frostbite and nerve palsy. The skin and underlying tissues cannot withstand freezing temperatures for extended periods. Therefore, you should always adhere to the 15 to 20-minute guideline to prevent harm.
Is 10 minutes long enough to ice?
For smaller areas or sensitive individuals, 10 minutes can be sufficient. If the injury is superficial, such as a finger or toe, 10 to 15 minutes is adequate. The cold penetrates these smaller areas much faster than large muscle groups. However, for a deep thigh bruise or a large joint, 10 minutes might not reach the target tissue effectively. In such cases, you may need the full 20 minutes.
How long after an injury can you put ice?
You should apply ice as soon as possible after the injury occurs. Immediate application yields the best results for controlling inflammation. Ideally, you want to start within the first five to ten minutes. The first 24 to 48 hours offer the most critical window for cryotherapy intervention. After 72 hours, the benefits of icing diminish as the body transitions to the repair phase.

Conclusion: Best Practices for Safe Recovery
Managing an injury effectively requires a blend of knowledge and patience. The application of ice remains a cornerstone of acute injury care. However, it must be performed correctly to be beneficial. We have established that timing is everything. As a general rule, you should apply ice for no more than 20 minutes at a time. You should repeat this every two to three hours during the initial 48-hour window. The question of how long should you ice an injury is not just about duration but also about technique. Always use a barrier like a towel to protect your skin. Furthermore, pay close attention to your body’s signals. If the area becomes numb or shows signs of frostbite, stop immediately.
Moreover, remember that ice is just one part of the larger recovery picture. The R.I.C.E. protocol provides a solid framework for initial care. Yet, as healing progresses, you must adapt your strategy. Transitioning to gentle movement and heat therapy facilitates tissue remodeling. Avoid the common mistake of over-icing, which can lead to further complications. Instead, monitor your symptoms closely. If swelling persists or pain worsens despite home treatment, seek professional medical advice. A doctor or physical therapist can provide a tailored rehabilitation plan. They can ensure that you are not exacerbating the issue. By following these guidelines, you can use cold therapy as a powerful ally in your recovery journey. You will heal faster and safer, getting you back to your normal activities with confidence.
